By Henrylito D. Tacio
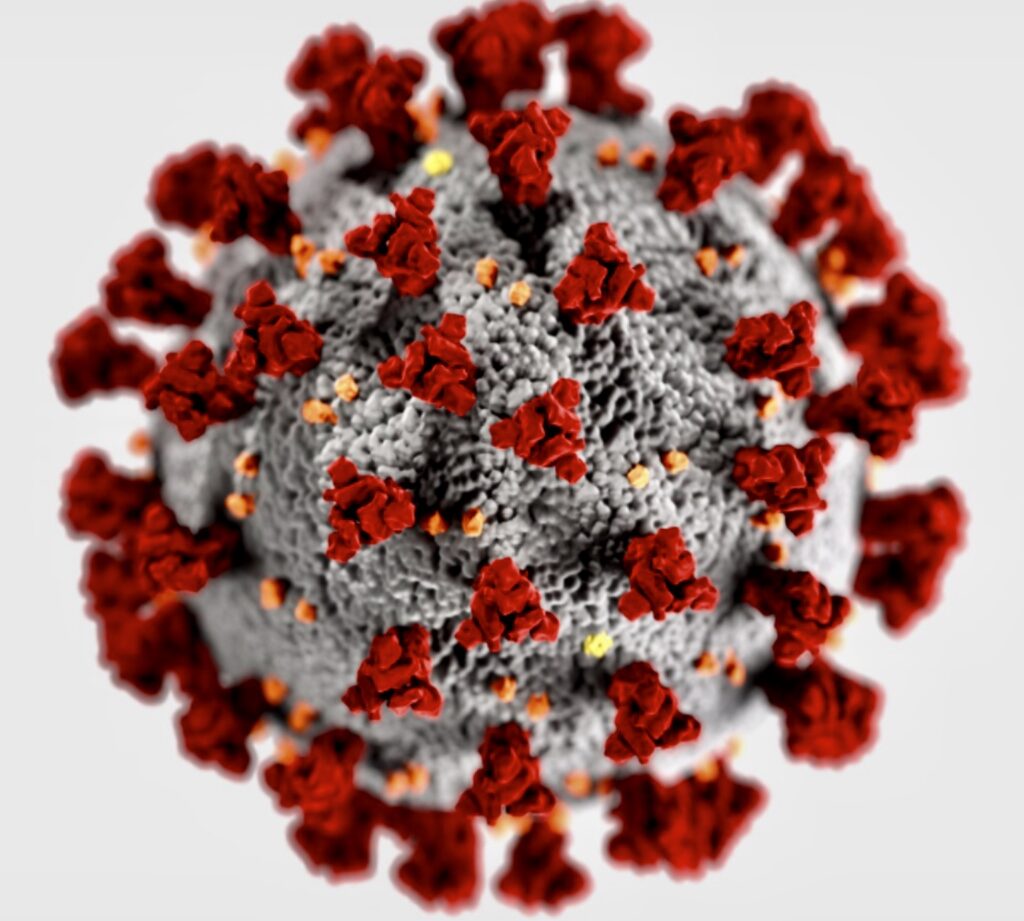
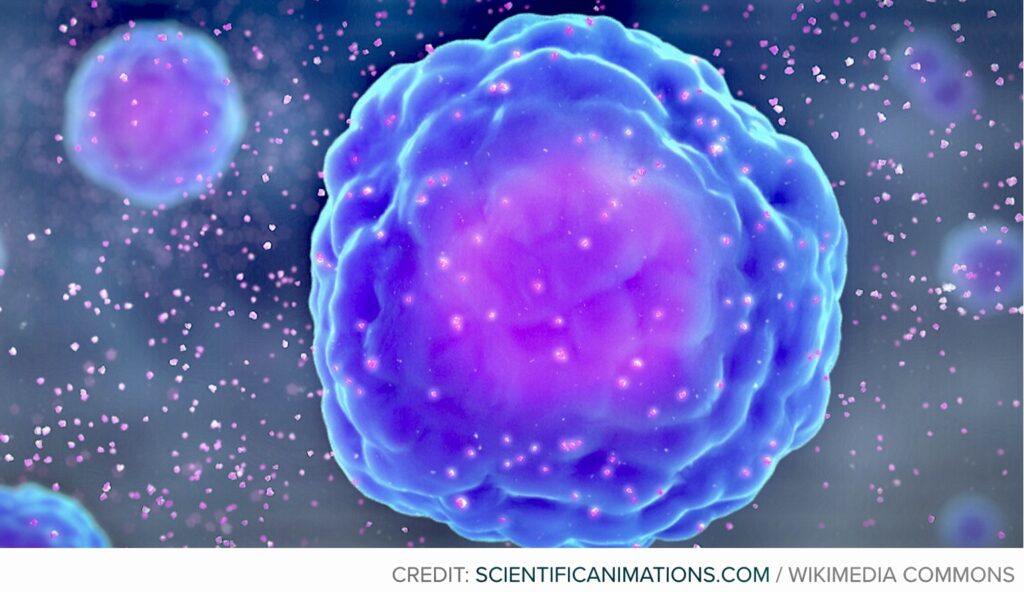
Photo credits: COVID-19 virus (from CDC), cytokine storm (from Scientificanimations.com), and RT-PCR lab (courtesy of WHO)
Despite the discovery of new medicines, there are still old drugs that can do wonders against new diseases. What medical scientists need to do is discover how these drugs can beat novel microorganisms creating havoc in a person’s body.
That is what the Canadian researchers were doing when they use a powerful anti-inflammatory drug to reduce the risk of pulmonary complications and death among those infected with a new coronavirus that is a distant cousin of Severe Acute Respiratory Syndrome called SARS-CoV-2.
SARS-CoV-2 has been identified as the microorganism that causes the coronavirus disease 2019 (COVID-19), which was first reported in Wuhan, China. By January 2020, the dreaded bug started to spread around the world. By March, the World Health Organization (WHO) declared it a pandemic.
According to the United Nations health agency, the most common symptoms of COVID-19 are fever, dry cough, and fatigue. Other symptoms that are less common and may affect some patients include loss of taste or smell, nasal congestion, conjunctivitis (red eyes), sore throat, headache, muscle or joint pain, and different skin rash types nausea or vomiting, diarrhea, and chills or dizziness.
Symptoms of severe COVID-19 include shortness of breath, loss of appetite, confusion, persistent pain or pressure in the chest, and high temperature (above 38°C). Other less common symptoms are irritability, confusion, reduced consciousness, anxiety, depression, sleep disorders, and more severe and rare neurological complications such as strokes, brain inflammation, delirium, and nerve damage.
Studies done on the novel coronavirus showed some patients to have had several complications from a surge of activated immune cells in the lungs, which is called in medical parlance as “cytokine storm.”
“When the cytokines that raise immune activity become too abundant, the immune system may not be able to stop itself,” explains Amber Dance in an article that appeared in Knowable Magazine. “Immune cells spread beyond infected body parts and start attacking healthy tissues, gobbling up red and white blood cells, and damaging the liver.
“Blood vessel walls open up to let immune cells into surrounding tissues, but the vessels get so leaky that the lungs may fill with fluid, and blood pressure drops,” Dance continues. “Blood clots throughout the body, further choking blood flow. When the organs don’t get enough blood, a person goes into shock, risking permanent organ damage or death.”
With this information, a Canadian team led by Jean-Claude Tardif, director of the Montreal Heart Institute research center and professor of medicine at the University of Medicine, conducted a study on the drug colchicine, hoping that it will work to moderate the overproduction of immune cells and their activating compounds in COVID-19 patients.
Colchicine is used to prevent or treat the symptoms of gout, which is caused when a substance called uric acid forms painful crystals in the body, typically in the joints. The oral tablet is available as both a generic and brand-name drug. It also comes in capsules that are also available as both a generic and brand-name drug.
To conduct the clinical study, the team started looking for people who had been infected with COVID-19 “in the past 24 hours who are 40 years or older, and who are not hospitalized.”
The institute called the clinical research COLCORONA, which commenced in March 2020. The objective was “to determine whether short-term treatment based on colchicine would reduce the risk of pulmonary complications and death related to COVID-19.”
“More specifically, COLCORONA studies the phenomenon of major inflammatory storms present in adults suffering from severe complications related to COVID-19,” the institute added.
The COLCORONA study – described as “a contact-less, randomized, double-blind, placebo-controlled clinical trial that took place at home” – was also conducted in the United States, Europe, South America, and South Africa.
Last January 22, the institute released the findings of the research. “The study results have shown that colchicine has reduced by 21% the risk of death or hospitalization in patients with COVID-19 compared to placebo,” the Globe Newswire reported. “This result obtained for the global study population of 4,488 patients approached statistical significance.
“The analysis of the 4,159 patients in whom the diagnosis of COVID-19 was proven by a naso-pharyngeal PCR test has shown that the use of colchicine was associated with statistically significant reductions in the risk of death or hospitalization compared to placebo,” Globe Newswire added.
In the patients with a proven diagnosis of COVID-19, colchicine reduced hospitalizations by25%, the need for mechanical ventilation by 50%, and deaths by 44%. “This major scientific discovery makes colchicine the world’s first oral drug that could be used to treat non-hospitalized patients with COVID-19,” the institute said.
In a press conference, Dr. Tardif echoed the same reassuring statement: “Our research shows the efficacy of colchicine treatment in preventing the ‘cytokine storm’ phenomenon and reducing the complications associated with COVID-19. We are pleased to offer the first oral medication in the world whose use could have a significant impact on public health and potentially prevent COVID-19 complications for millions of patients.”
The institute hopes that prescribing colchicine to COVID-19 patients “could help alleviate the problems of hospital congestion and reduce healthcare costs around the world.”
Before you buy colchicine, there are some things you need to know, according to the website healtline.com. Although the oral tablet doesn’t cause drowsiness, it has side effects, including pain in the abdomen (stomach area), constipation, diarrhea, nausea, and vomiting.
Its serious side effect is rhabdomyolysis (muscle damage) which can cause kidney disease and can be life-threatening. Symptoms can include muscle weakness and muscle pain.
Colchicine may also interact with other medications like antifungal drugs, HIV drugs, antibiotics, and antidepressants. Among the interactions that can increase the risk of side effects include cholesterol drugs, Digoxin (an antiarrhythmic drug), heart drugs (particularly verapamil and diltiazem).
People with allergic reactions to colchicine should not take it. Symptoms of a severe allergic reaction include trouble breathing and swelling of the throat or tongue. “Don’t take this drug if you’ve ever had an allergic reaction to it,” healthline.com warns. “Taking it again could be fatal (and may cause death).”
For people who are suffering from gout and taking colchicine, healthline.com raises some important warnings:
Overdose warning: “Taking too much colchicine can be serious enough to cause death. Never take more of this drug than your doctor prescribes.”
Blood disorders warning: “Colchicine may cause your body to produce fewer blood cells of different types. This could raise your risk of infection or bleeding because some of these blood cells fight infection and help form blood clots.”
Muscle damage warning: “Colchicine can damage your muscles if you take it for 6 months or longer. Your risk is higher if you’re a senior. Taking other drugs that cause muscle damage, such as cholesterol medications, may increase this risk.”