Text and Photos by Henrylito D. Tacio
Additional Photo: Getty Images
China first reported a novel coronavirus that wreaked havoc in Wuhan in 2019. The World Health Organization (WHO), based in Geneva, called it coronavirus disease 2010 (COVID-19) and the virus that causes it SARS-CoV-2 as it is a distant cousin of Severe Acute Respiratory Syndrome virus.
“We have enough of these lockdowns and community quarantines,” said Generoso, a mechanic who has six children. “Our income is getting less and the food on our table is affected. Time will come when we don’t have anything to eat anymore.”
He is not alone. Thousands, if not millions, of Filipinos, are now suffering because of this COVID-19 threat. There is no end at sight.
Now, there are thousands of different types – or variants – of COVID-19 circulating around the world. The most famous ones are Alpha (B.1.1.7), first identified in the United Kingdom; Beta (B.1.351), first identified in South Africa; Gamma (P.1), first identified in Brazil; and Delta (B.1.617.2), first identified in India.
Now comes the Lambda variant (C.37), which was first detected in December 2020 and was given the name by the United Nations health agency in June 2021. “As the Delta variant ravages across communities in Asia, Europe, and the United States, another variant, Lambda, is spreading rapidly throughout South America,” said Forbes in a report written by William A. Haseltine, a professor at Harvard Medical School and Harvard School of Public Health.
In the Philippines, the first case of Lambda variant – that of a 35-year-old female case – was reported last August 15. The patient, according to the Department of Health (DOH), was “asymptomatic and tagged as recovered after undergoing the 10-day isolation period.”
“Change is the only permanent thing in this word,” said the Greek philosopher Heraclitus. And viruses are no exception, including SARS-CoV-2. “Most changes have little or no impact on the virus’ properties,” the WHO explains.
“However, some changes may affect the virus’s properties, such as how it easily spreads, the associated disease severity, or the performance of vaccines, therapeutic medicines, diagnostic tools, or other public health and social measures,” the WHO adds.

Wearing face mask 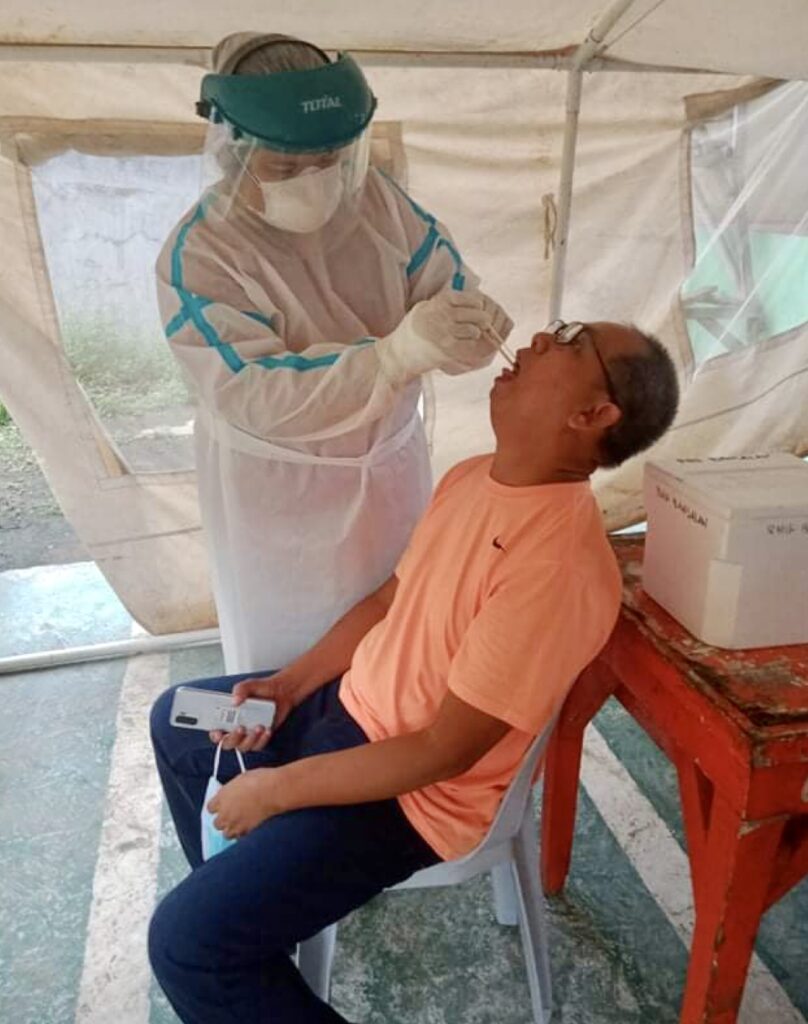
Swabbing
Given the continuous evolution of the virus that leads to SARS-CoV-2 and the constant developments in the understanding of the impacts of variants, the CDC has come up with a variant classification scheme: variant of concern (VOC) and a variant of interest (VOI).
A variant is considered of concern when there is evidence of an increase in transmissibility, more severe disease (that is, increased hospitalizations or deaths), a significant reduction in neutralization by antibodies generated during previous infection or vaccination, reduced effectiveness of treatments or vaccines, or diagnostic detection failures.
It’s a variant of interest when the variant with specific genetic markers has been associated with changes to receptor binding, reduced neutralization by antibodies generated against previous infection or vaccination, reduced efficacy of treatments, potential diagnostic impact, or predicted increase in transmissibility or disease severity.
The WHO currently designated four variants as VOC: Alpha, Beta, Gamma, and Delta. There are four VOI: Eta (detected in several countries in December 2020), Iota (first reported in the United States in November 2020), Kappa (also from India, first reported in October 2020), and Lambda (first reported in Peru in December 2020).
Right now, Delta is making headlines around the world due to its extra-transmissibility. According to the US Centers for Disease Control and Prevention (CDC), the Delta variant is more than twice as transmissible as the original strain of the coronavirus.
Peru has been hit hard by the Lambda variant, as 97 percent of its COVID-19 cases were Lambda. Reports said that for every 100,000 people in the population, 596 of them have died of COVID-19.
Lambda, like Delta, has now gone globetrotting as it has been reported in South America (Brazil, Chile, Colombia, and Ecuador), North America (the United States and Canada), Europe (France, Germany, Israel, Spain, and United Kingdom), Africa (Zimbabwe) and 18 other countries.
“Lambda has been associated with substantive rates of community transmission in multiple countries, with rising prevalence over time concurrent with increased COVID-19 incidence,” the WHO said.
Last June, the UN health agency declared Lambda a “global variant of interest.” In England, the Public Health office designated it a “variant under investigation” because of its “international expansion and several notable mutations.”
According to respected scientists, Lambda has this “unusual combination” of mutations, which makes it more transmissible.
“Lambda has seven mutations on the spike protein, the mushroom-shaped projections on the outer shell of the virus that help it latch onto our cells and invade them,” explains Tara Hurst in an article she writes for The Conversation. “These mutations may make it easier for lambda to bind to our cells and make it harder for our antibodies to latch onto the virus and neutralize it.
But before you jump into a conclusion, here’s what Hurst adds: “But it’s important to remember that neutralizing antibodies aren’t the only tool in the immune system’s toolkit –they are merely the easiest to study. T-cells play a vital role, too, so a handful of mutations – however unusual – might not be enough to allow lambda to dodge our immune system altogether.”
Right now, there are still no published studies on the Lambda variant. At hand are only a handful of preprints, or those papers that have yet to be subject to the scrutiny of other scientists (peer review) and published in a journal.
Two highly publicized laboratory studies from Japan and Chile – in preprint and unpublished yet – have suggested that “Lambda may be more infectious and less susceptible to current vaccines than the original coronavirus.”
“New findings have shown that vaccines such as Pfizer, Moderna and CoronaVac are less effective on Lambda than on the original, but are still tough enough to neutralize the variant,” wrote Sara Kiley Watson in an article published in popsi.com and based her report from a preprint from the New York University Grossman School of Medicine. “But there is still a lot to learn.”
CCN quoted Dr. Preeti Malani, the chief health officer in the division of infectious disease at the University of Michigan in Ann Arbor, saying that controlling the spread of COVID-19, in general, will help manage the Lambda variant.
“It’s a race between getting enough of the world vaccinated and the development of new variants that are less responsive to countermeasures,” Dr. Malani pointed out.
Scientists from all over the world seem to agree. In fact, they believe that in order for these mutations to stop, the world’s population has to be vaccinated against COVID-19. “As long as a significant portion of the world’s population remains unvaccinated or without immunity to the coronavirus, it will keep mutating and more variants will form,” writes Jessica Rendall for cnet.com.
Meanwhile, the emergence of the Lambda variant has made Dr. Kevin Kavanagh, a member of the editorial advisory board of Infection Control Today, to consider vaccines just one layer of protection against COVID-19 infection. People should combine vaccination with face masks and face shields. “Our goal needs to be to prevent both death and long-term disability,” he says.