AORTA DISSECTION: WALKING TIME BOMB
By Henrylito D. Tacio
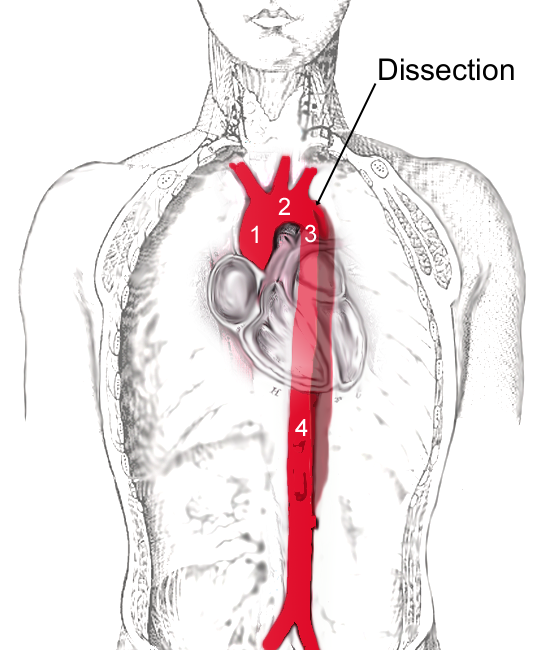
Illustration from Wikipedia
On September 11, 2003, Hollywood actor John Ritter fell ill while rehearsing for the television comedy, 8 Simple Rules for Dating My Teenage Daughter. He started sweating profusely, vomiting, and complained of having chest pains.
The television actor was immediately taken across the street to the Providence Saint Joseph Medical Center. Unfortunately, physicians misdiagnosed Ritter and treated him for a heart attack. As a result, his condition worsened.
Later, the doctors diagnosed Ritter with an aortic dissection. But at 10:48 pm, six days before his 55th birthday, the actor who rose to fame via Three’s Company, died during surgery to repair the dissection.
Although it is only about one inch in diameter, the aorta is the largest artery of the body. “It receives oxygen-rich blood from the left ventricle and distributes it to all of the body except the lung (which receives blood from the right ventricle),” explains The Merck Manual of Medical Information.
“Just after the aorta leaves the heart, smaller arteries that carry blood to the head and arms branch off,” the Merck manual continues. “The aorta then arches down, with additional smaller arteries branching off along its route from the left ventricle to the lower abdomen at the top of the hipbone (pelvis). At this point, the aorta divides into the two iliac arteries, which supply blood to the legs.”
When the lining of the aorta tears, blood can surge through, causing the middle layer of the wall to separate (dissect) from the still intact outer layer. As a result, a new, false channel forms in the wall of the aorta.
Aortic dissection results in a weakened blood vessel. Once this happens, “the weakened blood vessel may burst, which usually results in death if not treated immediately,” cautions WebMd.com.
The WebMd.com cites the following as probable causes of aortic dissection:
High blood pressure: Most patients with an aortic dissection have had high blood pressure for several years. The high blood pressure accelerates the natural processes of tissue aging and damage to the tissue, promoting a weakness of the aortic wall and increasing the risk for a tear.
Processes associated with high blood pressure: Medical conditions associated with high blood pressure also increase the risk of developing an aortic dissection. These include pregnancy, lupus, polycystic kidney disease, temporal arteritis, cocaine abuse, and abuse of stimulants. In pregnancy, the increased frequency of aortic dissections is caused by the combination of hormonal effect on the blood vessel wall and additional high blood pressure stress. High-intensity weightlifting and other strenuous resistance training may increase risk of aortic dissection by increasing blood pressure during the activity.
Diseases of the connective tissue: The most common is Marfan’s syndrome, a condition in which connective tissue, which supports various structures in the body, is weak. People with this disorder often have a family history of aneurysms of the aorta and other blood vessels. Other connective tissue disorders include Ehlers-Danlos syndrome, a group of connective tissue disorders characterized by skin that bruises or tears easily, loose joints and fragile blood vessels; and Loeys-Dietz syndrome, with twisted arteries, especially in the neck.
Chest injury: Severe chest injury, such as might occur in an automobile accident, may also cause aortic dissection.
The Mayo Clinic classifies aortic dissections into two groups, depending on which part of the aorta is affected: Type A and Type B. The former is more common and dangerous as it involves a tear in the part of the aorta where it exits the heart or a tear in the upper aorta (ascending aorta), which may extend into the abdomen. Type B, on the other hand, involves a tear in the lower aorta only (descending aorta), which may also extend into the abdomen.
“The condition most frequently occurs in men in their 60s and 70s,” the Mayo Clinic informs. “Symptoms of aortic dissection may mimic those of other diseases, often leading to delays in diagnosis. However, when an aortic dissection is detected early and treated promptly, the chance of survival greatly improves.”
Virtually everyone who has an aortic dissection experiences pain. “A sudden onset of pain is typical at the moment of dissection. The pain is usually described as ripping or tearing and as the worst pain ever experienced. It is usually in between the shoulders on the back and might radiate to the arms or the neck. Less frequently, the pain can be felt as chest pain. The pain is very difficult to distinguish from that of angina or a heart attack,” WebMd.com points out.
According to the Mayo Clinic, aortic dissection symptoms may be similar to those of other heart problems, such as a heart attack. Aside from sudden severe chest or upper back pain, other symptoms include loss of consciousness, shortness of breath, and sudden difficulty speaking, loss of vision, weakness or paralysis of one side of your body, similar to those of a stroke.
There is a lack of pulse in most instances. “In about two-thirds of people with aortic dissection, pulses in the arms and legs are diminished or absent,” the Merck manual informs.
The Merck manual says that as dissection advances, it can close off the points at which one or more arteries branch off from the aorta, blocking blood flow. “The consequences vary depending on which arteries are blocked,” it says. “Consequences include stroke (if the cerebral arteries, which supply the brain, are blocked), heart attack (if the coronary arteries, which supply the heart muscle, are blocked), sudden abdominal pain (if the mesentery arteries, which supply the intestines, are blocked), lower back pain (if the renal arteries, which supply the kidneys, are blocked) and nerve damage that causes tingling or inability to move a limb (if the spinal arteries are blocked).”
Blood may leak from the dissection and accumulate in the chest. “Blood leaking from a dissection near the heart may enter the pericardial space (between the two layers of membranes that surround the heart), preventing the heart from filling properly and causing cardiac tamponade — a life-threatening disorder.”
In a way, aortic dissection is a life-threatening disorder. “Around 1 in 5 patients with aortic dissection die before reaching the hospital. Without treatment, the mortality rate is 25% in one day, 50% in one week, 75% in one month, and 90% in three months,” writes Dr. Willie T. Ong, an active consultant in cardiology at the Manila Doctors Hospital and Makati Medical Center.
“When the patient reaches the hospital, the mortality rate is about 30% for a dissection of the ascending and thoracic aorta, and 10% for the abdominal aorta,” Dr. Ong continues.
“For the patients who survive the acute episode, survival rate is around 60% in 5 years and 40% in 10 years.”
Acute aortic dissection can be treated medically or surgically. “Since the most crucial factor that favors dissection is the systolic blood pressure (the first number of the blood pressure), doctors prescribe drugs called beta-blockers to decrease the force of the heart’s pumping,” Dr. Ong says.
According to Dr. Ong, surgery may be needed in complicated cases, such as blockage in the arteries of the limbs, persistent pain, and ballooning of the aorta with danger of a full-blown rupture. “That is why this condition is sometimes called a ‘walking time bomb’ since we don’t know when the rupture will occur,” he says.
“All people who have aortic dissection, including those treated surgically, have to take drug therapy for the rest of their lives,” the Merck manual reminds. “Such therapy helps reduce stress on the aorta.”