Written By Henrylito D. Tacio
“The solution to (COVID-19) is just around the corner. All we need to do is awake the energy in our midst.” – Dr. Jeffrey M. Ramos, Diving, Hyperbaric Medicine and Difficult Wounds Unit, Department of Emergency Medicine at Southern Philippines Medical Center
***
Before 2019 ended, a novel coronavirus was traced to a food market in Wuhan, China. At the beginning of 2020, it generated headlines all over the world because of “the unprecedented speed of its transmission.”
From China, the virus has reached countries as far as the United States and the Philippines. Today, the pandemic has become “the worst crisis of this generation” as it not only a health issue but an economic matter as well.
The World Health Organization (WHO) officially called it SARS-CoV-2, as it is a distant cousin of the coronavirus that causes Severe Acute Respiratory Syndrome. The disease was named COVID-19, which stands for coronavirus disease in 2019.
The most common symptoms of COVID-19, according to the United Nations health agency, are fever, dry cough, and fatigue. Other symptoms that are less common and may affect some patients include loss of taste or smell, nasal congestion, conjunctivitis (also known as red eyes), sore throat, headache, muscle or joint pain, different types of skin rash, nausea or vomiting, diarrhea, and chills or dizziness.
However, some develop severe symptoms like shortness of breath, loss of appetite, confusion, persistent pain or pressure in the chest, and high temperature (above 38⁰C). There are those who experience confusion, anxiety, depression, sleep disorders, and reduced consciousness (sometimes associated with seizures).
“Among those who develop symptoms, most (about 80%) recover from the disease without needing hospital treatment,” the WHO says. “About 15% become seriously ill and require oxygen and 5% become critically ill and need intensive care.”
Complications leading to death may include respiratory failure, acute respiratory distress syndrome (ARDS), sepsis and septic shock, thromboembolism, and/or multiple failures, including injury of the heart, liver, or kidneys.
As of November 24, Davao City has 5,881 confirmed cases of COVID-19. So far, 3,601 have recovered with 263 deaths (that’s about a 4.5% case fatality rate).
Most of those who died have experienced severe COVID-19 and have co-morbidity, defined as the presence of one or more additional conditions often co-occurring with the primary condition. This means that aside from COVID-19, the patient may be suffering from diabetes, asthma, hypertension, and other health problems.
But there are those who suffer severe COVID-19 – and yet live to tell their story. Take the case of 40-year-old Mario (not his real name), who was admitted to the Southern Philippine Medical Center (SPMC) in Davao City on October 25.
Still single and living with his parents, he was brought to the hospital because he was suffering from severe acute respiratory illness with difficulty in breathing, symptoms of the dreaded disease.
The Department of Internal Medicine diagnosed him with having a severe COVID-19 with comorbidity of obesity, hypertensive cardiovascular disease, and coronary artery disease.
Immediately, Mario was given the necessary treatments. He was started on compassionate treatment of antivirals, steroids, and anticoagulants. Based on the daily monitoring of the patient’s blood markers and clinical manifestations, relative to the course of his disease, he was not improving but instead he was getting worse.
The doctors decided to do something to save the patient’s life. On the fourth day, when his inflammatory and mortality markers were at its worst, he was referred to the Diving, Hyperbaric Medicine, and Difficult Wounds Unit of the SPMC’s Department of Emergency Medicine. There, he was given the hyperbaric oxygen (HBO2) therapy.
All in all, Mario had a total of eight sessions. “There was an immediate improvement in mortality markers, and clinical manifestation was evident right after the first hyperbaric oxygen treatment session,” reports Dr. Jeffrey M. Ramos, who is with the DEM’s Diving, Hyperbaric Medicine and Difficult Wounds.

On the 12th day of his admission at the hospital and the last of his HBO2 treatment, Mario finally recovered. He was already independent from oxygen supplementation and can breathe freely on his own with no difficulty.
“The patient subjectively reported to us that his difficulty in breathing was improving immediately after the first hyperbaric treatment session,” Dr. Ramos explains. “He was already relieved in the eighth session.
“Blood parameters also showed alleviation from hypoxia as evidenced by his arterial blood gas monitoring, and consistent progressive improvement with his inflammatory, and mortality markers on a daily basis,” he continues. “Chest X-rays also showed significant improvement as well.”
Two days later, or on the 14th day since he was admitted, Mario was released from the hospital and went back to his home. “Doc, I will return here to thank you since the treatment you have given me saved my life,” he told Dr. Ramos.
Since COVID-19 hit the country beginning March this year, medical authorities have a hard time finding possible solutions to the pandemic. Since it was a new disease, they have to resort to trial and error methods. There are no specific treatments. Doctors compare notes and treatments.
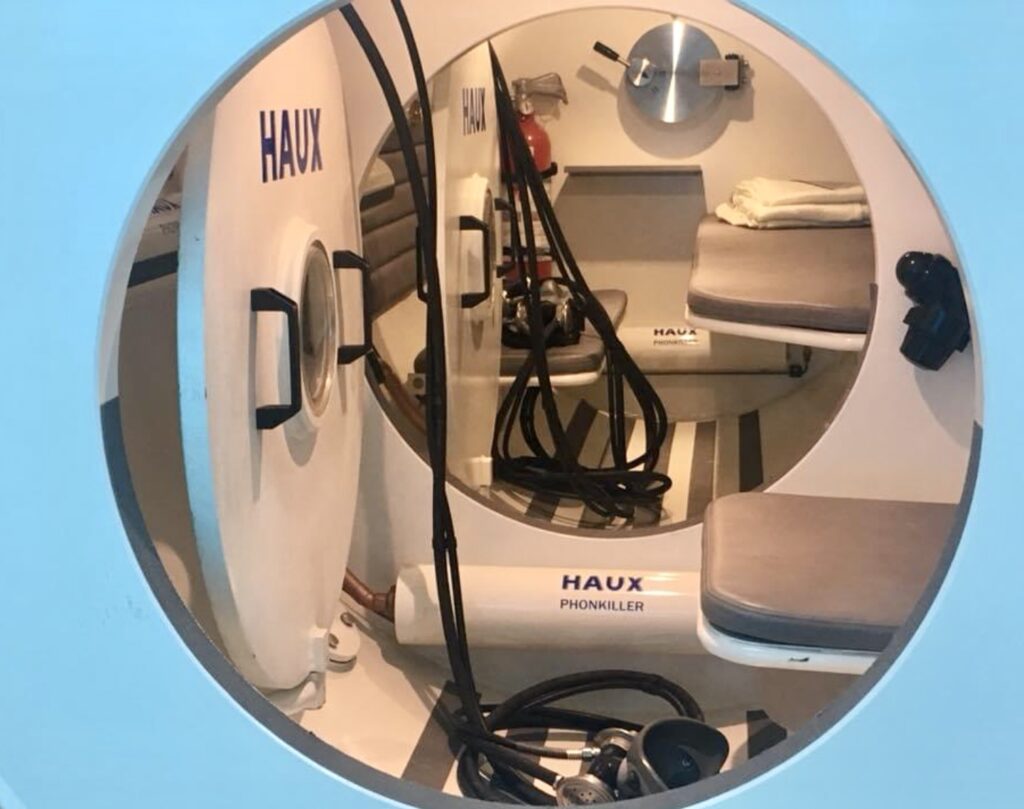
The HBO2 is a new thing in treating COVID-19. The Undersea Hyperbaric Medical Society (UHMS) defines HBO2 as “an intervention in which an individual breathes near 100% oxygen intermittently while inside a hyperbaric chamber that is pressurized to greater than sea level pressure (1 atmosphere absolute).”
Here’s how it works, according to Medical News Today’s Yvette Brazier: “The body’s tissues need oxygen to function, and additional oxygen can help damaged tissue heal. Oxygen at high pressure can enhance tissue function and fight infection under certain conditions.
“The ambient pressure inside the chamber is three times higher than the air pressure that people normally breathe,” Brazier continues. “Breathing almost pure oxygen at this pressure can increase the concentration of oxygen available to the lungs by up to three times.”
The SPMC was the first to implement such an initiative in its quest to find treatment for severe COVID-19 cases. As Dr. Ramos discloses in an exclusive interview, “The genesis of the compassionate hyperbaric treatment protocol was a response to the health threat unleashed by the COVID-19.”
According to Dr. Ramos, death from COVID-19 is due to the effects of hypoxia (the condition in which “the body or a region of the body is deprived of adequate oxygen supply at the tissue level” , hyperinflammatory state (called in medical parlance as cytokine release storm), and hypercoagulable state (“a condition in which there is abnormally increased tendency toward blood clotting”).
“These complications can be mitigated by hyperbaric oxygen therapy, thereby decreasing the risk of having the patient deteriorate to the critical state (which leads to high percentage of mortality) of the COVID-19 spectrum,” Dr. Ramos points out.
The establishment of the protocol was conceived in April 2020. It was only in September 2020 that the doctors were able to institute the compassionate use hyperbaric treatment to the first patient. “We hope to conclude the study early next year,” Dr. Ramos said.
Currently, the SPMC itself is funding the study. Aside from Dr. Ramos, the following are also involved in the study: Dr. Arthur R. Salvador, Dr. Jessa Javier-Ong, Dr. Faith Joan Gaerlan, Dr. Benedict Edward P. Valdez, Dr. Leopoldo J. Vega, Dr. Muhammad Mohamad, Dr. Neil Ramos, and Dr. Romulo Uy.
On why these doctors opted to study HBO2 as an adjunctive treatment against COVID-19, Dr. Ramos explains: There is no other way to increase blood plasma oxygen significantly other than hyperbaric oxygen therapy. Since COVID-19 can induce low blood oxygen level (hypoxemia) because of a diseased lung, it is rational that HBO2 therapy can help correct it. We also felt we have the expertise in this field of Hyperbaric Medicine, together with the Emergency Medicine and Pulmonology Section of the Internal Medicine as well as our hyperbaric certified nursing staff. We have the important equipment which is the mono-place hyperbaric chamber and complete life support and emergency equipment and most of all we have the proximity to the COVID 19 patients admitted.”
Among all the health institutions in the country today, the SPMC is the only establishment to have crafted a Compassionate Hyperbaric Treatment Protocol for COVID-19 with strict adherence to the UHMS and Infection Control Committee guidelines on instituting hyperbaric oxygen therapy on COVID-19 patients.
In addition, the SPMC is the country’s only institution to initiate, and organize a sub-specialty fellowship training program for Diving, Hyperbaric Medicine, and Difficult Wounds under the Department of Emergency Medicine, with well credentialed specialists.
Aside from Mario, there were other four cases – who suffered from severe COVID-19 – that fully recovered and are now living comfortably. “They were all sent home, recovered and free from complications, and are quite thankful for our service,” Dr. Ramos informs.
The success of the HBO2 treatment has encouraged SPMC doctors to have it further tested or implemented in the country. “With our 5 COVID-19 severe patients (take note, they are all severe) showing the same trends of improvement as soon as after the completion of the first session, and an untainted safety profile, who wouldn’t (recommend it)? We would even subject ourselves to this treatment if we catch ourselves some nasty COVID virus.”
Dr. Ramos ends the exclusive interview with these words: “We aim to institute this novel treatment modality to patients with moderate to severe COVID-19 in total enumeration. Hence, with the help of one of the co-authors of this protocol, who tirelessly facilitated the fast-tracking of our acquisition of the multi-place hyperbaric chamber (capable of treating 10 patients at one time), we can serve more patients.”

